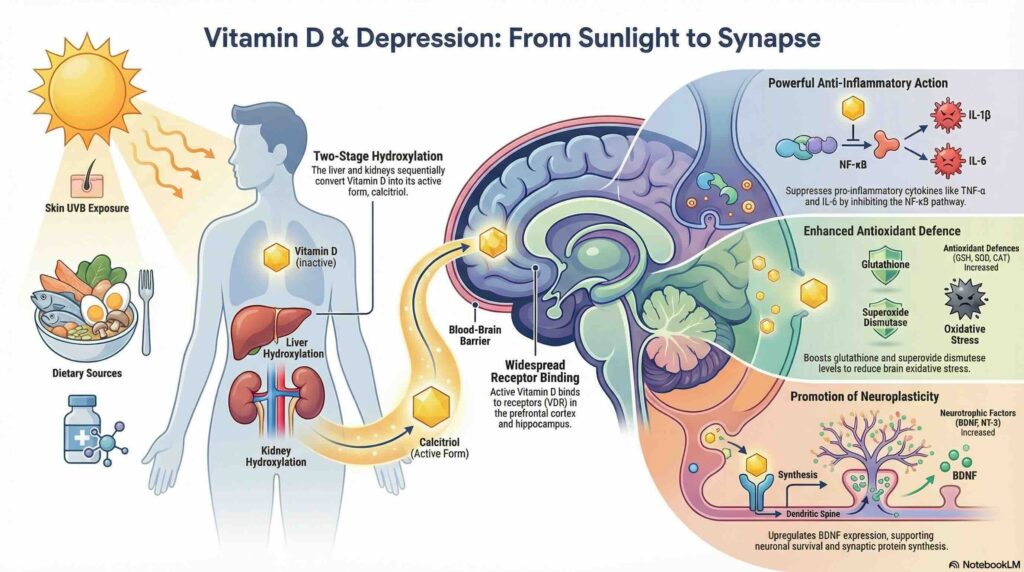
Introduction
The global burden of Major Depressive Disorder (MDD) remains one of the most formidable challenges in modern psychiatry, characterized by a biological complexity that spans genetic, environmental, and physiological domains. In a study published in the Journal of Steroid Biochemistry and Molecular Biology, titled “Vitamin D in major depressive disorder: Current evidence, possible molecular mechanisms, and future prospects,” Anderson Camargo and colleagues investigated the potential of vitamin D signaling to modulate the neurobiological pathways associated with this debilitating condition. This synthesis of preclinical evidence provides a rigorous framework for understanding how specific molecular targets might be harnessed to address persistent challenges in managing depressive symptoms.
Current pharmacological treatments for MDD are increasingly scrutinized for their limitations, particularly the significant time lag for clinical onset and the fact that approximately 30 percent of patients fail to respond to initial therapies. This clinical reality necessitates an urgent shift toward non-traditional therapeutic pathways that address the multifactorial etiology of the disorder. The development of depressive symptoms is closely linked to biological disruptions such as impaired neuroplasticity, chronic oxidative stress, and neuroinflammation. By evaluating these factors through the lens of vitamin D signaling, researchers are identifying a neuroactive and immunomodulatory system that extends far beyond traditional bone health to influence the very foundations of central nervous system function.
Audio Summary
Key Findings
Conclusion