Introduction
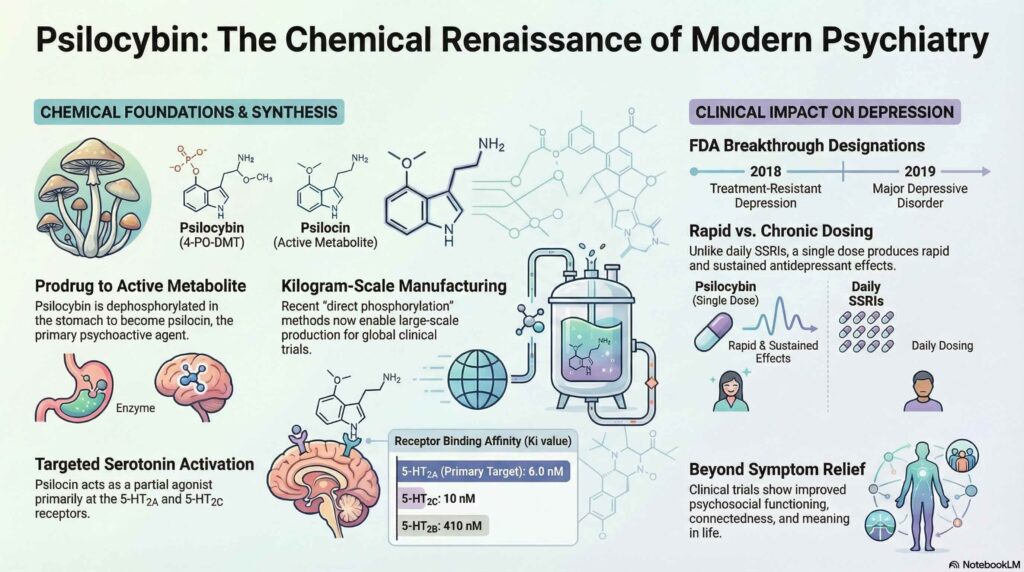
This mini-review explores the historical trajectory, chemical architecture, and biological mechanisms of psilocybin. Following its 1970 designation as a controlled substance, the field has entered a modern research renaissance. This shift is underscored by the FDA granting breakthrough therapy designations for Treatment-Resistant Depression (TRD) in 2018 and Major Depressive Disorder (MDD) in 2019. A central research question addressed is the technical challenge of establishing reliable, large-scale chemical synthesis to support expanding clinical trials and potential pharmaceutical integration.
Audio Summary
Key Findings
Psilocybin functions as a prodrug, undergoing rapid dephosphorylation in the stomach to become the pharmacologically active metabolite psilocin. This active form enters systemic circulation and crosses the blood-brain barrier to serve as a partial agonist at the 5-HT2A receptor. Beyond immediate sensory changes, psilocybin facilitates neuroplasticity by increasing extracellular concentrations of glutamate and dopamine in the frontal cortex. This neurochemical shift supports the rewiring of brain circuits and the reduction of neuroinflammation, providing a robust biological basis for its rapid and sustained effects on mood and cognitive function.
Clinical evidence suggests a single supervised dose can produce long-lasting antidepressant effects in patients with MDD and TRD. Beyond depression, the therapeutic horizon includes effective applications for anxiety and substance use disorders, such as nicotine and alcohol addiction. While generally well tolerated, side effects can include transient anxiety, nausea, and headaches. Real-world data indicates a 32.1% recurrence rate of psychedelic effects, or Hallucinogen Persisting Perception Disorder (HPPD). However, within the controlled environment of formal clinical trials, there have been no reported cases of HPPD as of November 2025.
Conclusion
This review details how sophisticated chemical synthesis and a clarified 5-HT2A mechanism are essential for the integration of psilocybin into modern psychiatric care. These developments facilitate the transition from laboratory curiosity to large-scale clinical feasibility. Future research must now determine if the subjective psychedelic experience is a prerequisite for therapeutic efficacy or if the underlying neurological adaptations can be triggered independently of the hallucinogenic trip.