Introduction
The traditional view of vitamin D as a narrow regulator of calcium and bone health is evolving toward a broader appreciation of its pleiotropic effects across multiple organ systems. During the 8th International Conference on Controversies in Vitamin D held in Rome, a multidisciplinary panel of experts sought to evaluate the hormone’s influence on gut homeostasis, infectious disease risk, and autoimmune regulation. This consensus statement synthesizes observational and interventional data to clarify whether maintaining optimal vitamin D status can support systemic health beyond the prevention of rickets and osteoporosis.
Audio Summary
Key Findings
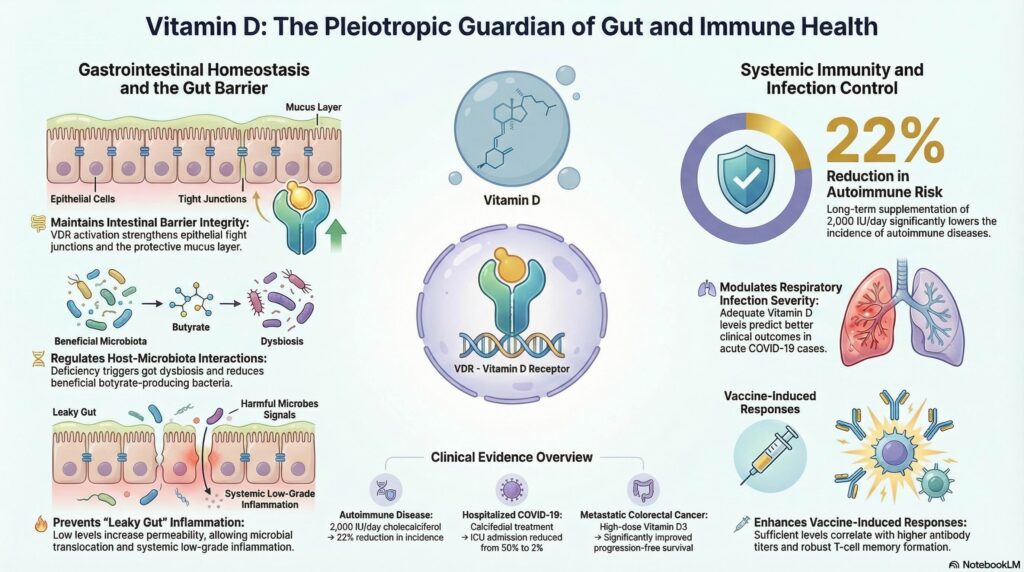
The Vitamin D Receptor (VDR) is essential for preserving the physical integrity of the intestinal barrier. Deficiency is associated with gut dysbiosis, which involves an imbalance of microbial communities and a specific reduction in beneficial butyrate-producing bacteria. These changes can impair the production of short-chain fatty acids, lead to a thinning of the protective mucus layer, and increase intestinal permeability. Such leaky gut conditions facilitate the movement of harmful substances into the bloodstream, potentially contributing to systemic low-grade inflammation and increasing the risk of colorectal cancer or complicating mucosal healing in patients with celiac disease.
Regarding infectious diseases, low levels of 25(OH)D are consistently linked to higher risks of respiratory infections and worse outcomes in COVID-19, though interpreting this data requires caution. An important clinical insight is that vitamin D may act as a negative acute-phase reactant, meaning circulating levels often drop as a direct result of systemic inflammation rather than being the primary cause of the illness. While large-scale trials of standard vitamin D3 have shown mixed results, specific interventions using calcifediol, a form of the hormone that bypasses hepatic processing for faster activity, have demonstrated potential in reducing intensive care admissions and mortality among hospitalized patients.
Vitamin D also supports central immune tolerance, which is the essential process by which the immune system learns not to attack the body’s own tissues. It plays a vital role in the thymus, the organ responsible for immune cell education, where a lack of vitamin D signaling is linked to disorganized architecture and the premature aging of the immune system. Clinical evidence from the VITAL trial initially showed that long-term supplementation was associated with a 22 percent reduction in autoimmune disease. However, scientific integrity requires noting that a subsequent analysis of the same cohort failed to confirm statistical significance and the protective effect appeared to wane after supplementation was discontinued.
Conclusion
These findings suggest that vitamin D functions as a multi-system regulator with implications for clinical practice far beyond bone density. While associations between vitamin D status and disease are strong, the evidence from interventional trials remains variable and highly dependent on baseline status and dosage. Given its high safety profile and low cost, the expert panel recommends maintaining vitamin D concentrations above 20 or 30 ng/mL for populations at skeletal or immunological risk. Optimizing these levels serves as a foundational strategy to support gut function and strengthen immune competence.