Introduction
The clinical world knows it as the “suicide headache.” It is an experience of neurological torture so visceral that it exists beyond the boundaries of standard medical description. For 15 to 180 minutes, a unilateral firestorm consumes the eye and temple, driving patients to bang their heads against walls or contemplate the finality of death just to escape the clockwork of their own brains. As both a researcher and a Cluster Headache (CH) warrior, I have long been haunted by a central research question: Why does this specific neurological cruelty seem to select for a very specific physical and psychological profile? Recent research, such as the work by Muñoz et al. (2016), suggests that those of us who carry this burden often share a distinct personality landscape.
The Leonine Mask: Physicality as Destiny

The Architecture of Suppression: “Anger-In”

The Leonine Mouse Paradox
When Relaxation Becomes a Trigger

The Paranoid-Schizoid Position: A Diagnostic Schism
Conclusion




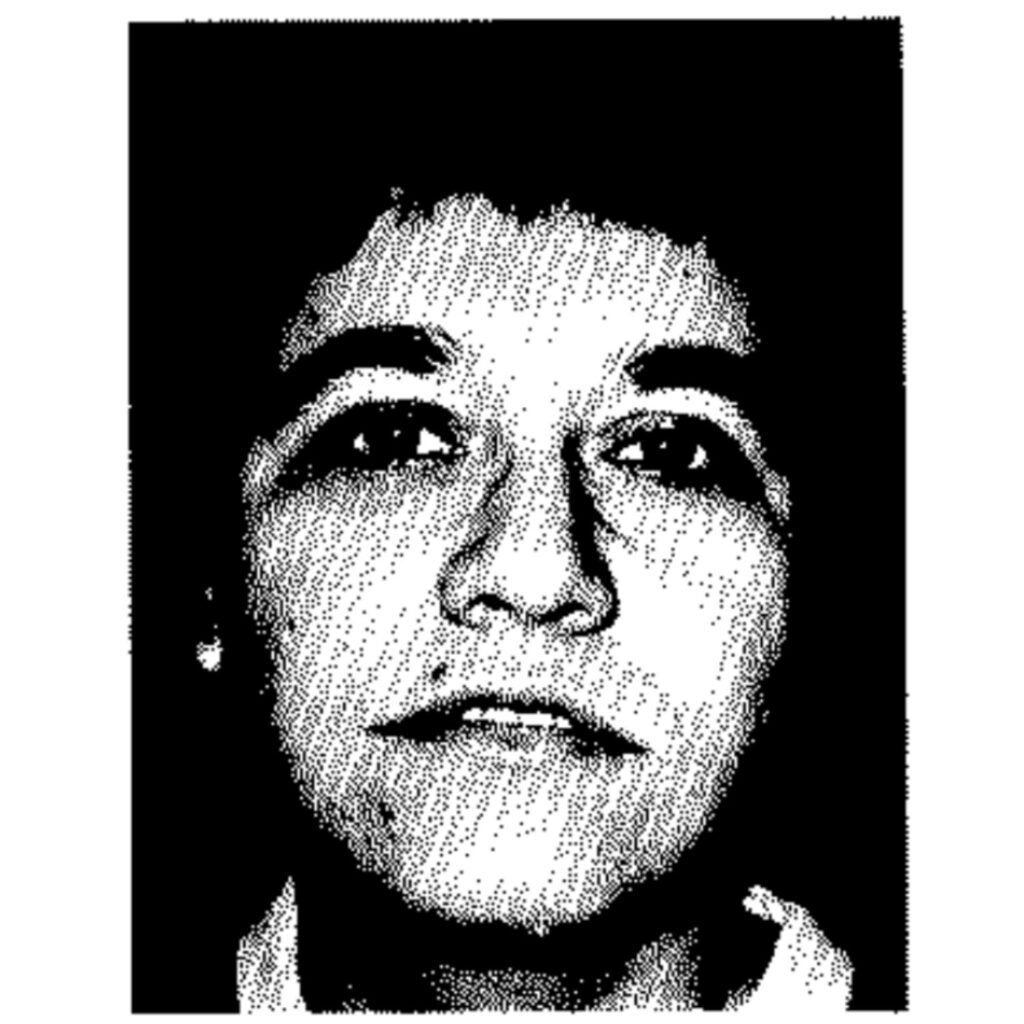



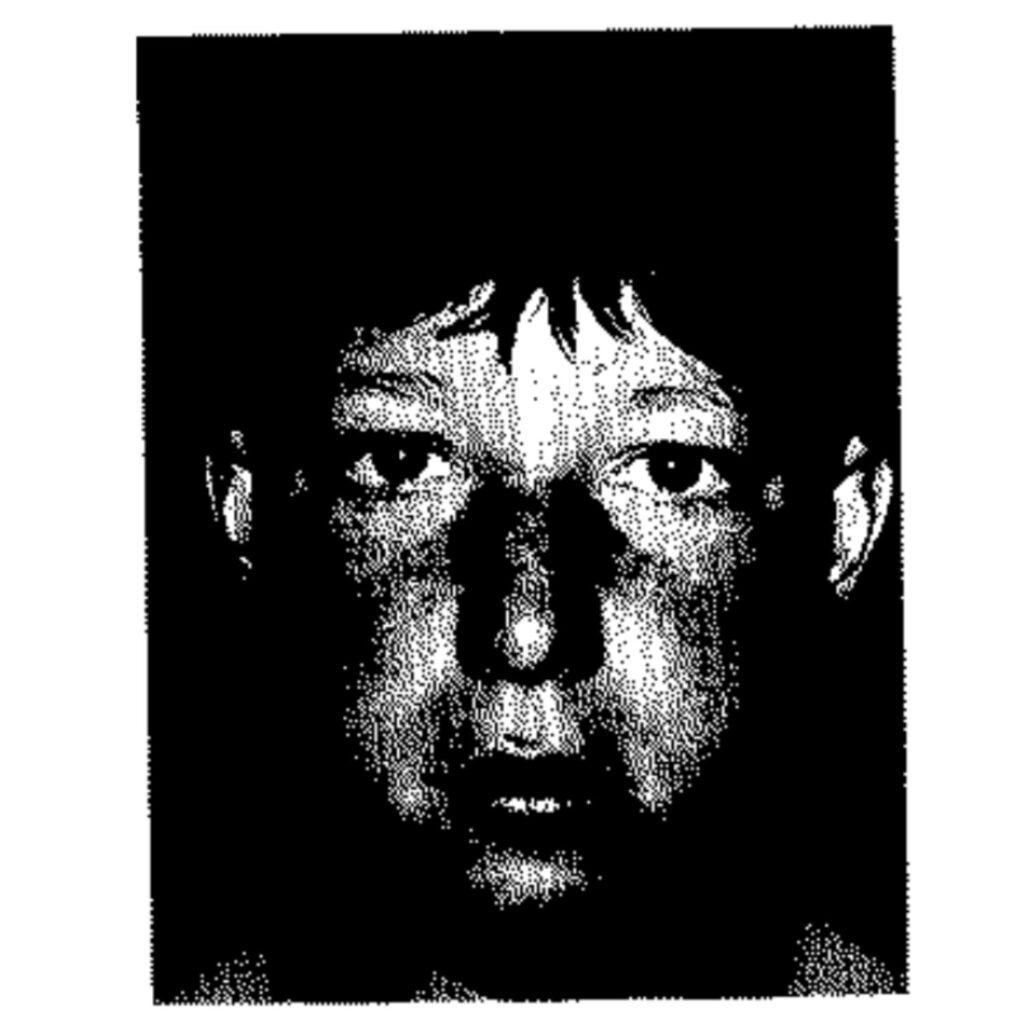
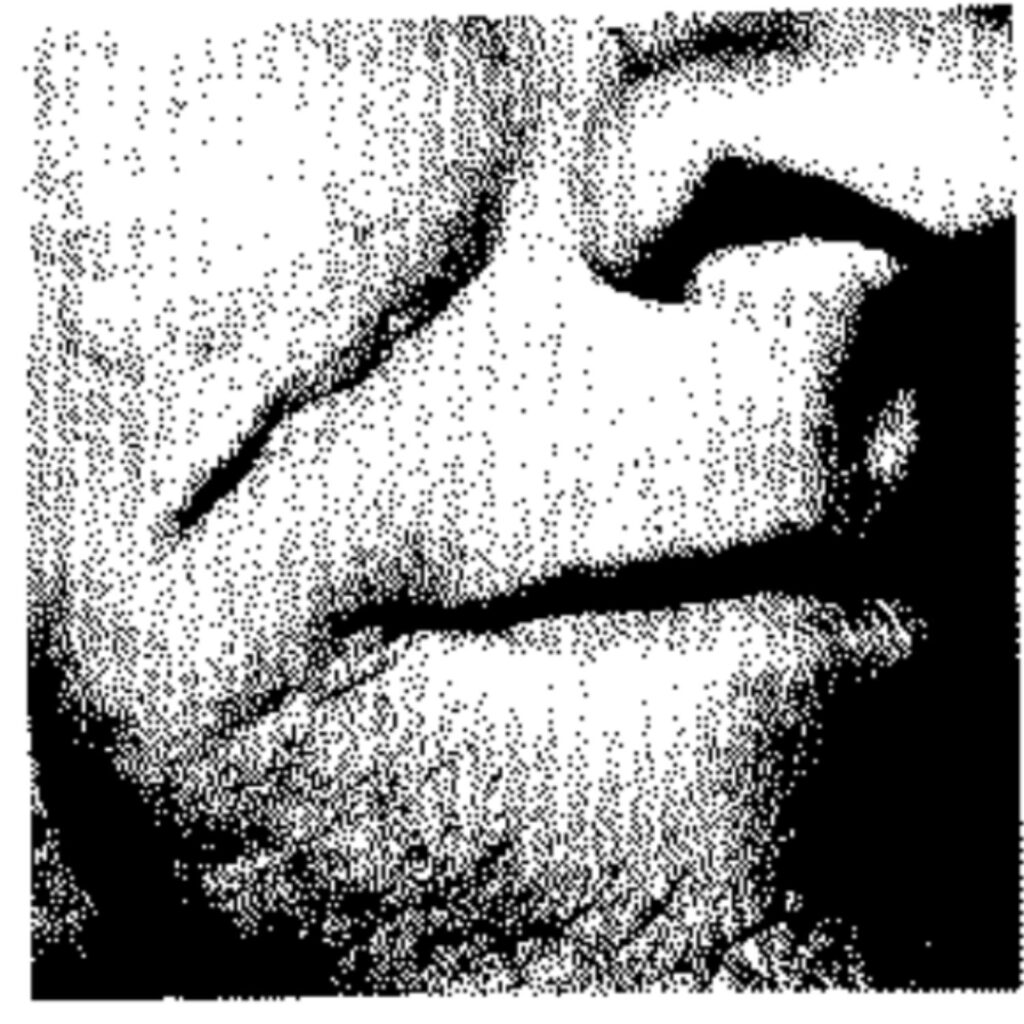

References
Cluster Headache. Headache Journal. 1972.
Cluster Headache. Postgraduate Medicine. 1974.
Cluster Headache: The Relation to Arousal, Relaxation, and Autonomic Tone. Headache Journal. 1990.
Physical and Personality Characteristics in Cluster Headache. Headache Journal. 1974.
The Seasonal Relationship of Cluster Headache. (Excerpts). 1987.