All Microbiome
- 2 mins to read
Migraine represents a significant global socio-economic burden, affecting around 14% of the population and ranking among the top causes of years lived with disability. Historically, management has been limited to reactive symptom suppression, but a strategic shift is now investigating the microbiome-gut-brain axis as a modifiable, upstream pathway for treatment. In a study published in Nutrients, titled “Migraine and the Gut-Brain Axis-The Role of Microbiome-Targeted Biotics,” Márk Kozák and colleagues investigated how biological modulation of the gut environment could redefine therapeutic outcomes. By pivoting from traditional pharmacology to the regulation of systemic pathways, this research evaluates how biotics may address
- 5 mins to read
Could the real trigger behind your migraines be hiding in your gut? In this article, we explore the emerging science behind the migraine gut connection, from microbial diversity deficits and leaky gut driven inflammation to disrupted serotonin pathways and CGRP activation. As research reshapes our understanding of migraine as a systemic gut brain disorder rather than a purely neurological glitch, a new question emerges: is restoring your microbiome the missing step toward lasting relief?
- 3 mins to read
In a profound departure from skeletal-only medicine, Professor Bruce Hollis and host Craig Stewart explore the transition of Vitamin D from a nutrient for bone health to a high-dose pharmacological tool. By examining the "8-day miracle" that halted Stewart’s cluster headaches, they reveal how autocrine signaling and specific co-factors are rewriting the rules of chronic disease management.
- 4 mins to read
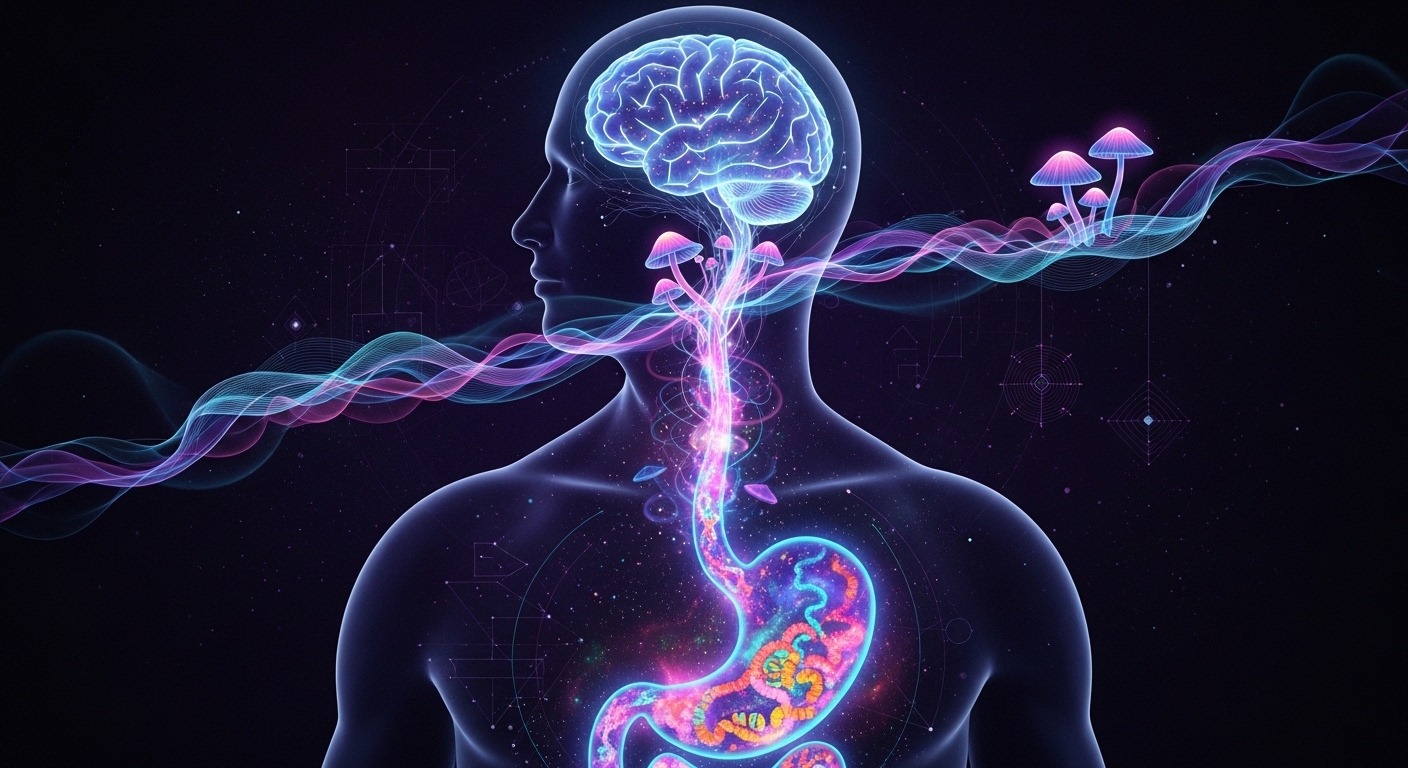
Psychedelic therapy is typically framed as a story of receptors, neurotransmitters, and neuroplasticity. Yet an emerging body of research suggests another protagonist may be quietly involved: the gut microbiome. Far from passive bystanders, microbial communities may influence how psychedelic compounds are metabolized, how inflammation is regulated, and why therapeutic responses vary so widely between individuals. This evolving gut-brain perspective invites a more integrative model of psychedelic efficacy, one that bridges psychopharmacology, immunology, and microbial ecology.
- 4 mins to read
The clinical divergence between high-cost monoclonal antibodies and the vitamin D3 anti-inflammatory regimen represents a critical evolution in the management of neurogenic inflammation. This analysis explores the molecular logic, physiological penetration, and genetic regulatory mechanisms that differentiate these two disparate neurological interventions.
- 4 mins to read
The efficacy of autoimmune treatment often hinges on the gut-immune-brain axis, where intestinal permeability induces a molecular blockade of Vitamin D utilization. This exploration details how restoring the microbiome can "renew" Vitamin D receptors, providing a roadmap to overcome enzymatic hijacking and therapeutic plateaus in cluster headaches and chronic autoimmune conditions.
Join the Community
Subscribe to receive updates on new research findings, articles and inspired conversations.
We respect your privacy. Unsubscribe at any time.