Introduction
Investigating CGRP-based therapies is a strategic necessity in CH care, where the limitations of traditional regimens are stark. While high-flow oxygen and triptans are effective for acute abortion, they do not address the frequency of attacks. Existing preventive agents like verapamil or topiramate are often hampered by slow onset and the requirement for transitional bridge therapy, such as prednisone, which carries its own side-effect profile. This study addresses the unmet need for targeted prevention by focusing on the role of CGRP. As a potent neuropeptide and endogenous vasodilator, CGRP is central to CH pathophysiology; its release from trigeminal afferent fibers during the activation of the trigeminal-autonomic reflex is a primary driver of the condition. By evaluating how CGRP blockade impacts these neural pathways, this meta-analysis yielded specific quantitative results regarding efficacy and safety.
Audio Summary
Key Findings
To establish a cohesive evidence base from a limited pool of large-scale studies, the research team performed a meta-analysis that integrated data from both randomized controlled trials and single-arm trials. This inclusive approach was necessary to maximize the available data, though it highlighted significant variability within the drug class. For instance, while agents like galcanezumab demonstrated substantial efficacy, others such as fremanezumab failed to meet clinical endpoints, leading to the early termination of its trials.
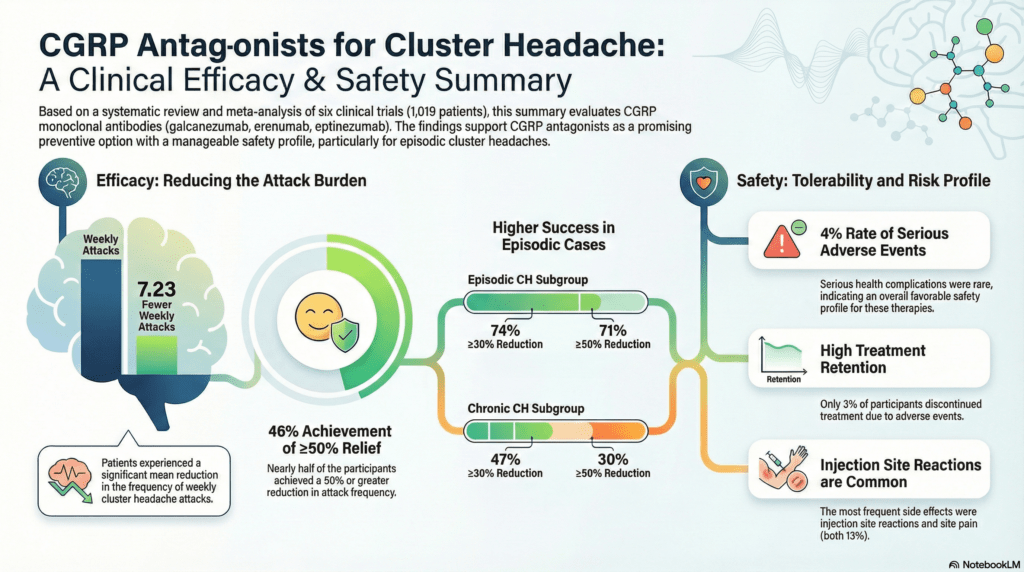
The analysis yielded several critical data points regarding the efficacy of CGRP antagonists:
• The mean reduction in the frequency of weekly attacks was -7.23.
• The 50% responder rate was 46%.
• The 30% responder rate was 59%.
• The Patient Global Impression of Change (PGIC) revealed that 42% of patients reported feeling much improved or very much improved.
The researchers observed a significant disparity in efficacy when comparing cluster headache subtypes. The treatment effect was notably larger in episodic cases, where the 50% responder rate reached 71%, compared to only 30% in chronic cases. This suggests that while episodic CH may be driven by transient CGRP-driven activation, chronic cases might involve additional central sensitization mechanisms. This phenomenon, where the central nervous system remains in a persistent state of high reactivity, appears less responsive to peripheral CGRP blockade alone.
Regarding safety, the profile of these antagonists was found to be acceptable and manageable. Approximately 60% of participants reported at least one treatment-emergent adverse event, though these were typically mild, such as injection site reactions. Serious adverse events were rare, occurring in only 4% of the population, and the discontinuation rate was low at 3%. Most importantly, the lack of vasoconstrictive properties in CGRP antagonists provides a clear safety advantage over traditional triptans, particularly for the middle-aged male demographic often affected by CH who may also carry higher cardiovascular risks.
Conclusion
These findings underscore the strategic value of incorporating CGRP antagonists into individualized treatment algorithms, potentially as a mechanism-based alternative or adjunct to agents like verapamil. By offering a targeted option, clinicians can better tailor prevention strategies to the specific needs of the patient.
While the results are encouraging, the researchers emphasize that the current body of evidence remains less definitive due to the limited number of available trials and the presence of significant statistical heterogeneity. The current findings should be viewed as supportive and hypothesis-generating rather than confirmatory. There is a measured call for the medical community to conduct larger, long-term, placebo-controlled trials to confirm these results and optimize therapeutic use. A concluding summary of the formal study parameters is provided below.