Introduction
Addressing lead migration is a primary strategic priority for the neurosurgical community, as the long-term viability of Occipital Nerve Stimulation (ONS) depends entirely on its mechanical stability. When electrodes shift from their intended position, therapeutic benefit is lost, forcing patients to undergo repeat surgeries that increase the burden on both the individual and the healthcare system. Historically, ONS adoption has been limited by high complication rates, necessitating the development of specialized hardware like the Ankerstim™ system, which is engineered specifically for the mobile anatomy of the neck.
The purpose of this study was to determine if ONS-dedicated leads, featuring integrated anchors and enhanced flexibility, could reduce the historically high rates of electrode migration observed with repurposed hardware. Chronic cluster headaches are frequently described as suicidal headaches because of their excruciating, relentless intensity, making a stable surgical solution a matter of life-altering necessity. Previous methods typically utilized spinal cord stimulation leads that were not optimized for cervical mobility, frequently resulting in displacement. This research evaluates outcomes within the French Occipital Nerve Stimulation Registry to determine if these technical advancements translate into sustained clinical safety.
Audio Summary
Key Findings
The results of this research mark a significant strategic advancement, proving that specialized hardware like the Ankerstim™ lead can bridge the gap between clinical effectiveness and surgical safety. By addressing the mechanical root causes of failure, the study demonstrates that dedicated engineering can stabilize the risk-to-benefit ratio for complex neuromodulation procedures.
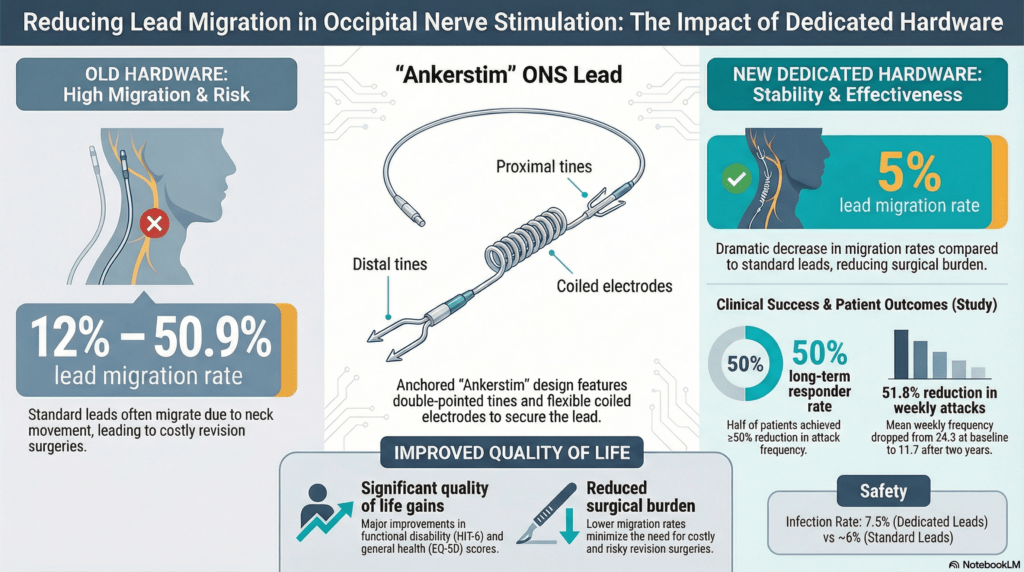
The primary data, following 40 patients at one year and 24 patients through two years, showed a profound reduction in hardware complications. The lead migration rate was only 5%, which stands in sharp contrast to the 12.9% to 50.9% migration rates reported in previous literature using non-dedicated leads. This improvement suggests that the integrated anchors and flexible design of the specialized leads successfully counteract the stresses caused by frequent neck movement.
The clinical impact on patient well-being was substantial, with the mean weekly attack frequency dropping from 24.3 at baseline to 11.7 at the two-year follow-up. These improvements were reflected in functional and emotional metrics, including the Headache Impact Test (HIT-6) and the Hospital Anxiety and Depression Scale (HAD-D). Notably, the study population reported baseline HAD-D scores that indicated clinical concern, as scores above 7 are significant, yet these scores improved as the attack frequency decreased.
While the specialized design improved stability, the study noted specific clinical trade-offs. A 12.5% rate of local pain was reported, often described by patients as a pulling sensation at the lead insertion site. Additionally, there is a technical balance between lead stability and the complexity of future removal. Because the leads are firmly anchored, extraction can be a surgical challenge, sometimes requiring a direct approach to the electrode tip and the use of intraoperative radiographic guidance for precise localization. Overall, the significant decrease in migration represents a fundamental shift in the safety profile of this technology.
Conclusion
These findings provide high strategic value for clinicians determining treatment pathways for patients who are refractory to standard care. By providing a more stable and reliable hardware option, ONS can be considered with greater confidence for those suffering from the extreme disability of chronic cluster headaches. The 5% migration rate achieved with dedicated leads directly mitigates the global burden and costs associated with revision surgeries, strengthening the case for the cost-effectiveness of this approach.
Within the scope of the French Occipital Nerve Stimulation Registry, these results indicate that while the effectiveness of the therapy remains consistent with previous methods, the improved safety profile represents a significant technical advancement. The reduction in lead migration addresses the most frequent criticism of ONS and supports its role as a viable, long-term intervention for rCCH.
Ultimately, these results suggest that dedicated hardware is the key to the maturation of peripheral nerve stimulation. However, the findings remain preliminary given the sample size and the impact of the COVID-19 pandemic on patient follow-up. Larger, long-term studies will be necessary to confirm these results and continue refining the surgical techniques required for these anchored systems.