Introduction
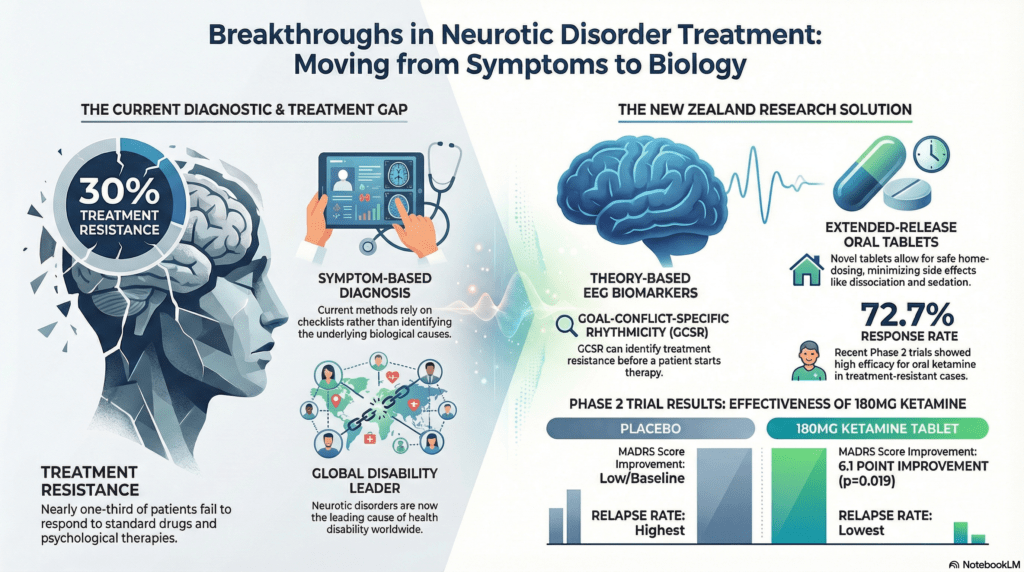
The primary purpose of this research is to move psychiatric diagnosis beyond its current reliance on symptom checklists, which lack the capacity to identify underlying biological causes. The authors compare the current diagnostic state of mental health to the hypothetical scenario of diagnosing COVID-19 solely through a list of symptoms, such as a cough or fatigue, rather than using a definitive biological test like a Rapid Antigen Test (RAT). By adopting the Research Domain Criteria (RDoC) approach, the study aims to move toward identifying syndromes based on pathophysiology to improve clinical outcomes. This is strategically vital because approximately 30% of patients with anxiety and depression are treatment resistant, failing to respond to at least two different drugs and psychological therapy. Developing theory-based biomarkers and novel treatments is essential to bypass the costly trial-and-error process that currently defines mental healthcare. These theoretical foundations, built upon 40 years of neuropsychological theory by Gray and McNaughton, have paved the way for measurable biological discoveries that could redefine the treatment landscape.
Audio Summary
Key Findings
The identification of Goal-Conflict-Specific Rhythmicity (GCSR) and the advancement of novel drug delivery methods are transformative for clinical outcomes because they allow for objective tracking of drug efficacy. By shifting toward precision psychiatry, clinicians can move away from unpredictable treatment cycles and toward targeted, data-driven interventions.
The researchers achieved a biomarker breakthrough by developing an EEG-based measure of GCSR. This rhythmicity is specifically sensitive to selective anxiolytic drugs, including benzodiazepines, buspirone, and pregabalin, with maximum individual power identified in the 4-7 Hz range. This discovery provides the first theory-based biomarker for a neurotic disorder, allowing researchers to isolate anxiolytic action neurally. Furthermore, the study evaluated the relationship between GCSR and treatment resistance. A significant finding revealed that while patients with anxiolytic-sensitive Generalized Anxiety Disorder (GAD) show high GCSR power, those with treatment-resistant GAD actually exhibit substantial negative GCSR. This distinction suggests that the biomarker can identify treatment resistance in advance, sparing patients from ineffective conventional therapies.
Simultaneously, a revolution in treatment is occurring through the use of ketamine. Research conducted across GAD, Social Anxiety Disorder (SAD), and Obsessive-Compulsive Disorder (OCD) has shown that low-dose ketamine can produce rapid and sustained improvements in symptoms. To make this treatment more accessible, Douglas Pharmaceuticals has developed an oral extended-release tablet. This formulation is designed to maximize active metabolites, specifically norketamine and hydroxynorketamine, which are more potent and detectable for longer periods than ketamine itself. This metabolic targeting helps minimize the dissociative side effects and blood pressure spikes often associated with injectable or intranasal delivery.
The clinical impact of these developments is substantial. In a phase 2 trial involving the extended-release tablets, 72.7% of patients were identified as treatment responders during the initial enrichment phase. Most of these individuals reported mood improvements within 48-72 hours of their first dose. The development of this tablet formulation is particularly significant as it may eventually facilitate home dosing, greatly expanding the number of patients who can access this therapy. These findings converge to shift the paradigm from trial-and-error to a future of precision psychiatry.
Conclusion
In medical research, measured and factual reporting is necessary to manage the expectations of both patients and healthcare providers. While the results regarding biomarkers and ketamine are promising, maintaining an objective perspective ensures that these tools are integrated into clinical practice responsibly and effectively.
For the future of New Zealand and international mental healthcare, these findings suggest a move toward the double hit hypothesis of neurotic disorders. This model posits that neuroticism is both a fundamental risk factor and a maintaining factor for various conditions. While conventional drugs might target specific traits, ketamine appears to act on the underlying neuroticism that drives the disorder. When supplemented with psychotherapy, such as Behavioral Activation Therapy (BAT), these biological interventions may provide more durable relief. Specifically, BAT is currently being studied to determine if it can prolong the positive benefits of ketamine after the active treatment period ends. The combination of objective EEG measures and practical oral delivery systems suggests a future where mental health treatment is faster, more effective, and more accessible.